What ECMO Feels Like From the Inside: Shane's Story
A note before you read
Shane wrote this himself. We did not change his words.
He went to bed one night with no reason to think anything was wrong. Hours later, he was in cardiac failure, on a ventilator, and then on ECMO, a machine that took over the work of his heart and lungs while his body tried to survive.
What follows is his account of what happened, what it felt like to wake up on the other side, and what he wishes he had known.
If your family member is currently on ECMO, some of what Shane describes may be familiar. Some of it may be hard to read. That’s okay. His story is not meant to predict what will happen to your loved one. Every case is different. But hearing from someone who has been there, in the bed, not beside it, can help you understand things that clinical explanations don’t reach.
Shane’s story:
I went to bed that night thinking about the next day and the coming weekend. Normal things. Ordinary plans. Nothing felt urgent. Nothing felt wrong enough to raise alarms. I had no reason to believe anything in my life was about to change.
Around midnight, I woke up and couldn’t breathe.
At first, I tried to work through it. Sitting up. Slowing my breathing. Telling myself it would pass. But it didn’t. Each breath felt harder than the last, like my body had suddenly forgotten how to do the one thing it had always done automatically. Eventually, Suzi, my partner at the time, called an ambulance.
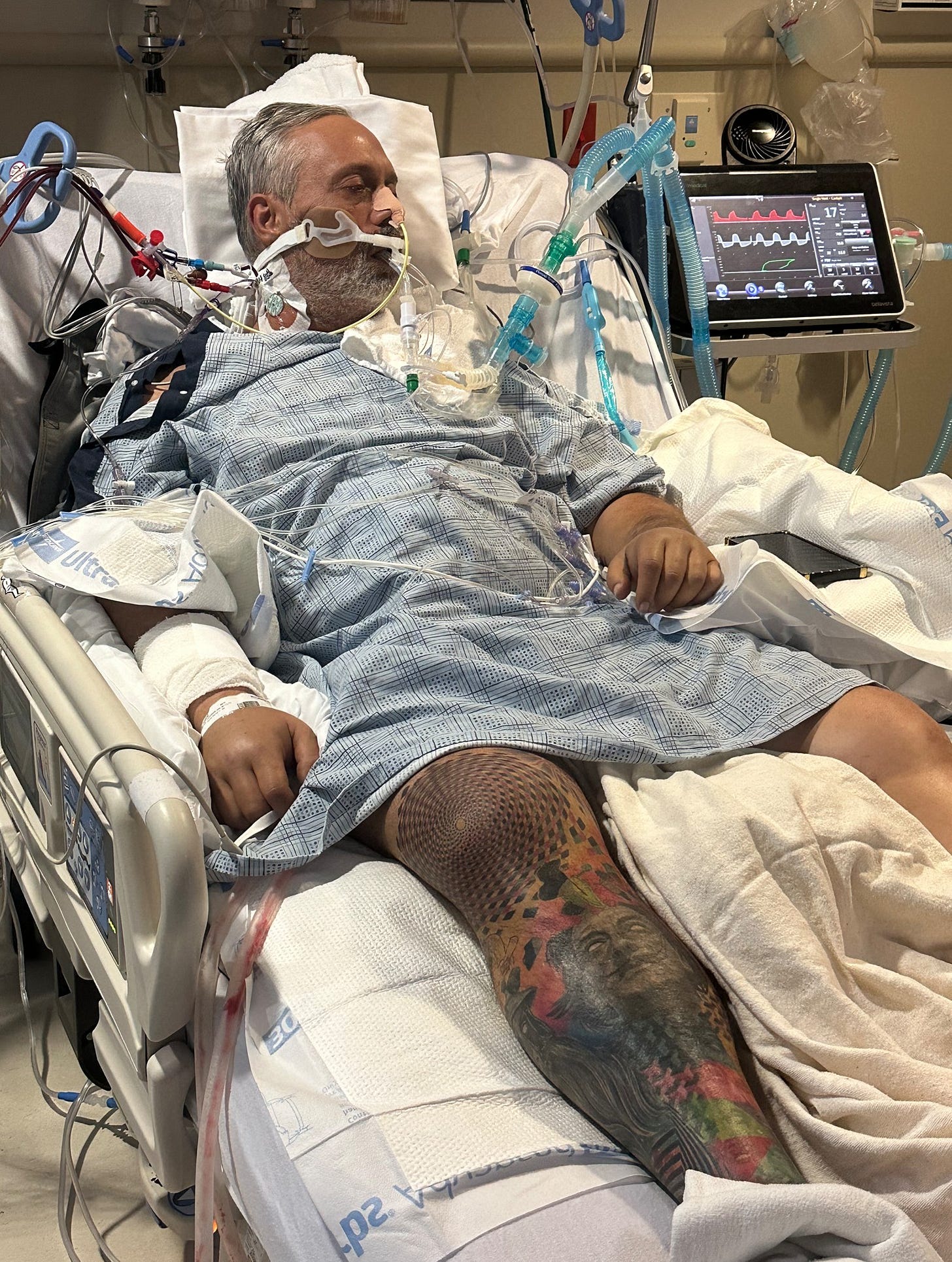
I later learned that when I arrived at the hospital, the medical team moved fast. Within a short time, I was placed on a ventilator and kept in a medically induced coma. My oxygen levels were critically low. My blood pressure was unstable and falling. My heart was failing. Teams of doctors and specialists were scanning my body, searching for answers and trying to stabilize me long enough to understand what was happening.
To keep me alive, I was placed on ECMO.
Everything at that stage was about buying time. I later learned that during surgery and resuscitation, the teams caring for me used medications called pressors to support my blood pressure. These drugs help redirect blood flow to the core and away from the limbs. They helped keep me alive, but they came at a cost.
I died on the operating table more than once when my blood pressure dropped before they got it back up. My kidneys failed after my heart stopped, and I was placed on continuous dialysis. I also developed severe swelling. Fluid leaked into places it shouldn't have, my body took on nearly 40 pounds of water, and my skin split open from the pressure.
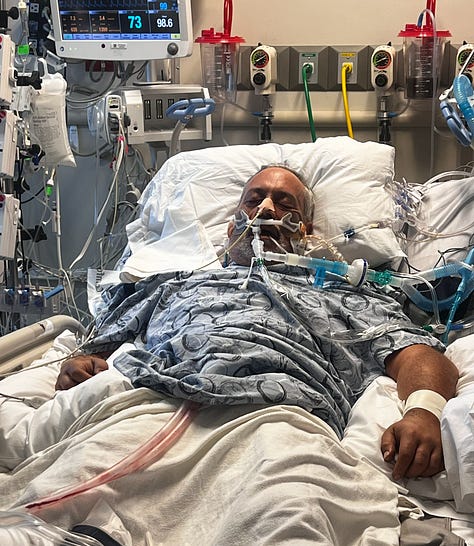
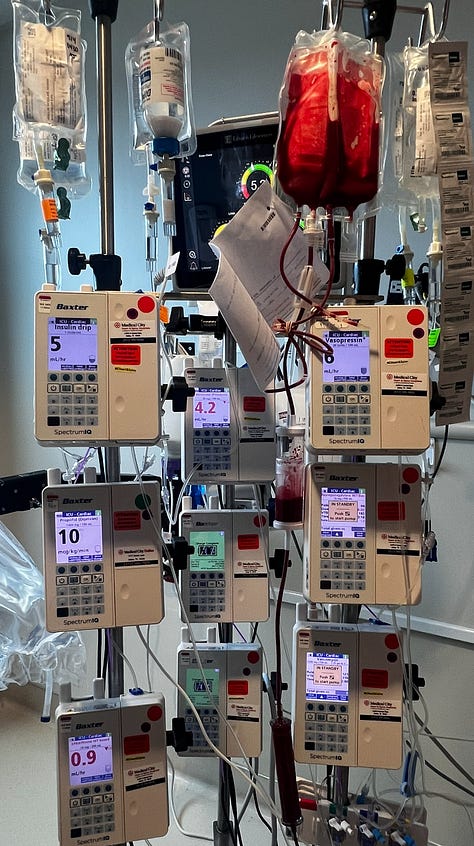
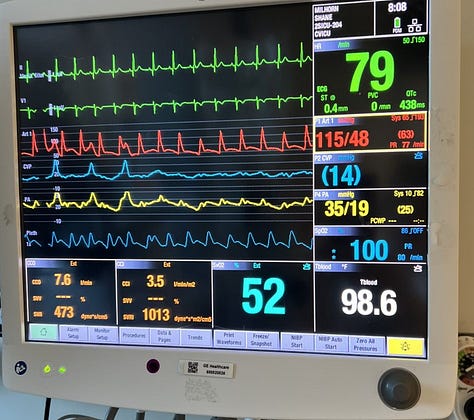
But even through all of that, they brought me back.
When I say “they,” I mean everyone involved. This was not one person or one team. It took every single person involved for me to be here today.
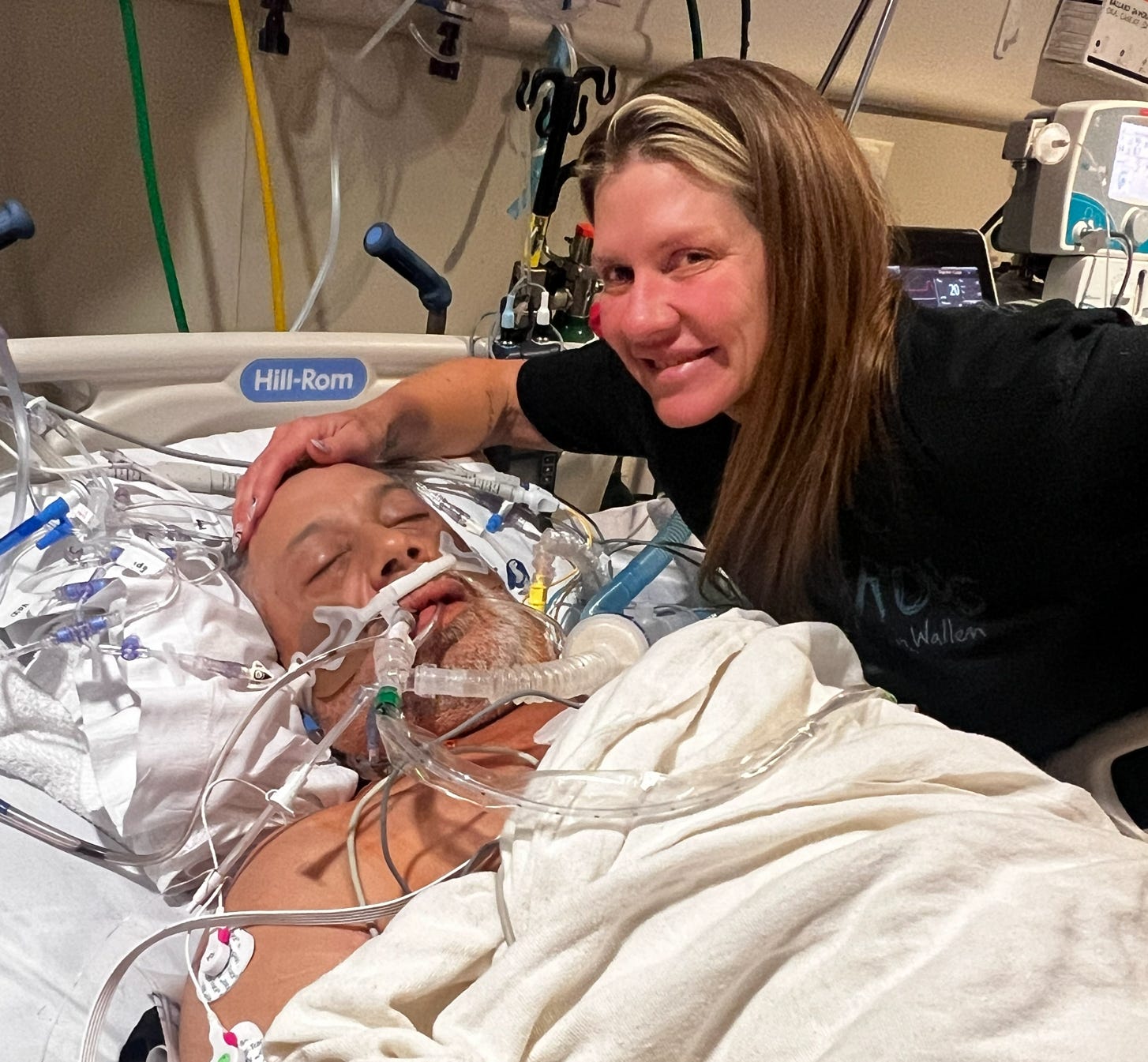
While I was unconscious, machines breathed for me and circulated my blood. I have no memory of any of it. Everything I knew from that time was told to me later.
What I do remember came after.
When I began to wake from the coma, nothing made sense. People spoke to me gently and slowly, trying to help, but it sometimes made it harder to process. I would lose track of what they were saying halfway through a sentence. It made me feel small, like I had lost something fundamental.
I couldn’t speak. I could barely move. I was whispering while confined to my bed, barely able to lift my arms or legs because of the weakness. My entire world had shrunk to a narrow strip of glass, about six feet by two feet and maybe eight feet high. The only thing I could really see was the sky.
I stared out that window constantly while doctors, specialists, nurses, family, and friends stood around me, speaking words I was not even sure I understood. I don’t even know when I fully realized what ECMO was. It was just a lot. A whole lot.
Two days after I woke up, they removed the ventilator. I had to relearn how to breathe on my own. Not figuratively. Literally. Every breath took effort. Every small gain felt massive.
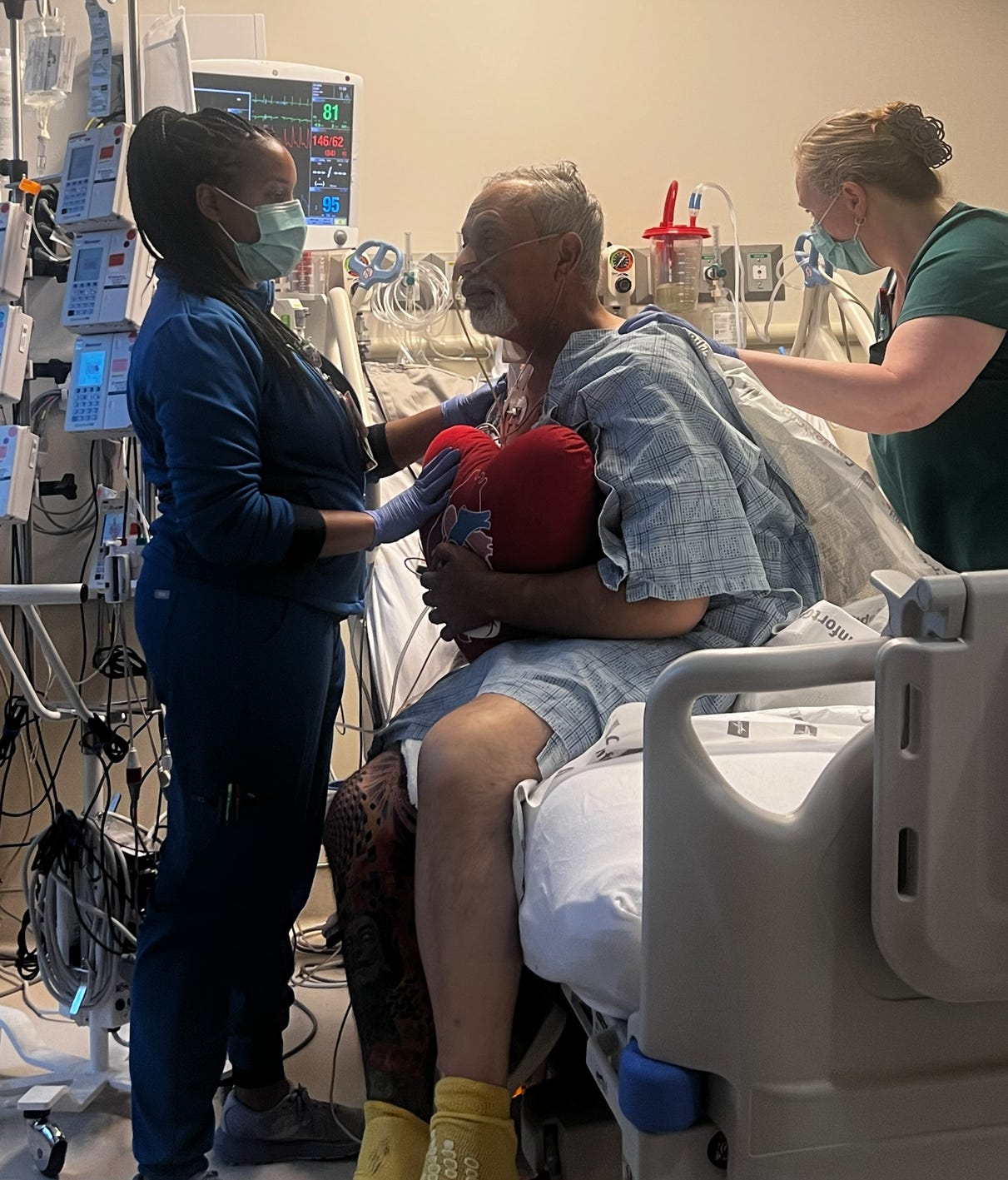
As my voice slowly returned, I had to rebuild my strength. Sitting on the edge of the bed, trying to keep my balance, felt overwhelming. The fear of failure was constant. So was the desire to get back to life. I remember the first day I stood up, my knees shaking, my body swaying, certain I was about to collapse. But I didn’t. I stood. Then, days later, I walked.
It’s incredible how much we take the simplest things for granted.
Over time, the reality of how close I had come to death began to settle in. I started to understand how much everyone had invested in keeping me alive. These people went through hell with me. They saw me knocking on death’s doorstep.
I didn’t want things handed to me anymore. I wanted to stand on my own. Walk on my own. Get my own ice. I needed them to know that their prayers, time, and energy were not in vain, that I was going to live the life they fought so hard to save.
Eventually, I was discharged.
But it wasn’t over.
I went home with both legs, but no one knew what would happen next. Eleven days later, the damage from the original event and the pressors caught up with me. The decision was made, and my leg was amputated. Once again, I was back in the hospital. Eight days later, I was released, and I have been moving forward ever since.
People ask me if ECMO, or this event in my life, changed me.
If I’m being honest, it did not change who I was. It confirmed it.
But there is something I believe deeply, and I want to be clear about it. No one comes back from something like this alone. Survival does not belong to one person. It belongs to the families who stayed, the friends who hoped, and the doctors, nurses, techs, specialists, and teams who never gave up, even while living through hell themselves and praying for a miracle.
One thing I wish I had understood sooner was the timeline. When ECMO happens, it happens fast. Once the immediate emergency passes, everything can feel vague and disorienting. As the patient, my mind was foggy, and I did not always know what questions to ask. That is where having an advocate mattered. Suzi asked what they were giving me, why they were doing it, and what each step meant. Those questions helped bring clarity in the middle of chaos, when everything was moving quickly, and understanding felt just out of reach.
A few things worth noting after you’ve read Shane’s story
Shane mentions several things in passing that deserve a brief explanation for families who are new to all of this:
Pressors are medications that tighten blood vessels to raise blood pressure when the heart can’t do it on its own. They can keep a person alive in a crisis, but they reduce blood flow to the limbs. In some patients, this contributes to tissue damage. Shane lost a leg to this, not to negligence, but to a brutal tradeoff the team had to make to keep him alive.
Third spacing means fluid leaks out of the blood vessels and collects in the body’s tissues. The body swells dramatically. Shane gained nearly forty pounds of fluid. This is alarming to see. It is a known complication of severe illness and major surgery.
Continuous dialysis is a slow, ongoing form of kidney support. When the kidneys stop working, as Shane’s did, this machine takes over, filtering waste from the blood around the clock.
Waking from a coma is not like waking from sleep. The brain has been heavily medicated and starved of normal stimulation. Many patients describe confusion, slow thinking, difficulty following words, and a sense of being trapped. Shane describes this clearly. It is common. It is temporary for most patients, though the timeline varies.
“One thing I wish I had understood sooner was the timeline. When ECMO happens, it happens fast. Once the immediate emergency passes, everything can feel vague and disorienting. As the patient, my mind was foggy, and I did not always know what questions to ask. That is where having an advocate mattered. Suzi asked what they were giving me, why they were doing it, and what each step meant. Those questions helped bring clarity in the middle of chaos, when everything was moving quickly, and understanding felt just out of reach.”
If you are in that waiting room right now, that is your job. Ask what each medication is for. Ask what each step means. You don’t need to understand everything — you just need to stay close to the information, because your loved one can’t yet.
Want to reach Shane?
Shane is open to hearing from survivors, family members, and anyone who wants to connect.
Email: stmillhorn@gmail.com