Understanding ECMO
An Overview for Patients, Family, and Friends
Key Points
ECMO (Extracorporeal Membrane Oxygenation): A life-support technique used for patients with severe heart and lung dysfunctions unresponsive to conventional treatments.
Functionality: ECMO temporarily takes over heart and lung functions by circulating blood outside the body through a machine that oxygenates it and removes carbon dioxide.
Types of ECMO:
Veno-Arterial (VA) ECMO: Supports both heart and lung functions.
Veno-Venous (VV) ECMO: Supports only lung function.
Indications for Use: ECMO is considered in cases of severe respiratory failure, cardiogenic shock, post-cardiac surgery recovery, and severe infections like pneumonia or COVID-19.
Risks and Complications: Potential risks include bleeding, infection, blood clots, and organ damage.
Understanding ECMO: A Comprehensive Overview
Extracorporeal Membrane Oxygenation (ECMO) is a specialized medical treatment that provides temporary support for patients with severe heart and lung dysfunctions. It serves as a bridge, allowing these vital organs time to rest and recover when traditional therapies are insufficient.
How Does ECMO Work?
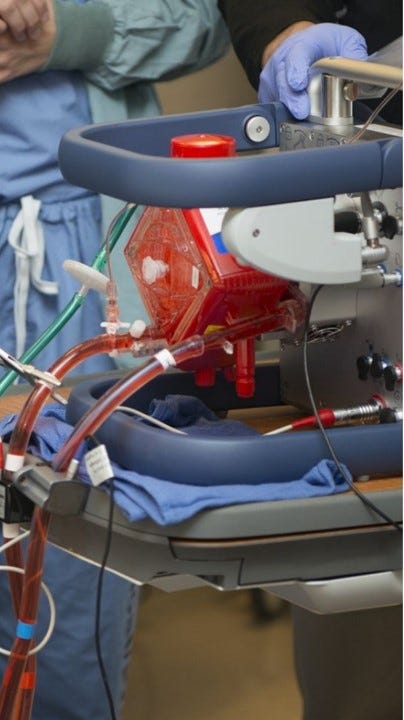
ECMO functions by diverting blood from the patient's body to an external machine that oxygenates it and removes carbon dioxide. This oxygen-rich blood is then returned to the body, effectively performing the roles of the heart and lungs. The primary components of the ECMO system include:
Cannulas: Flexible tubes inserted into large blood vessels to transport blood to and from the ECMO machine.

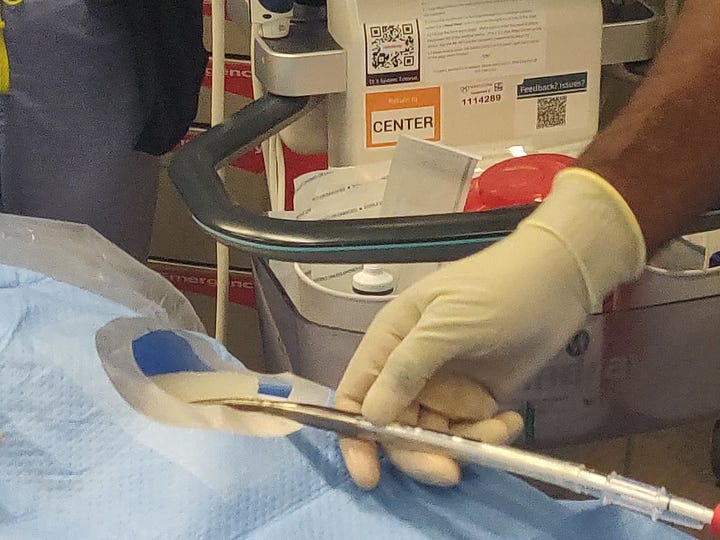
on the left is the cannula that gets insert into the patient. A lot of times into the groin or in a neck vien Pump: Acts as an artificial heart, propelling blood through the circuit.
Oxygenator: Serves as an artificial lung, adding oxygen to and removing carbon dioxide from the blood.
There are two main types of ECMO:
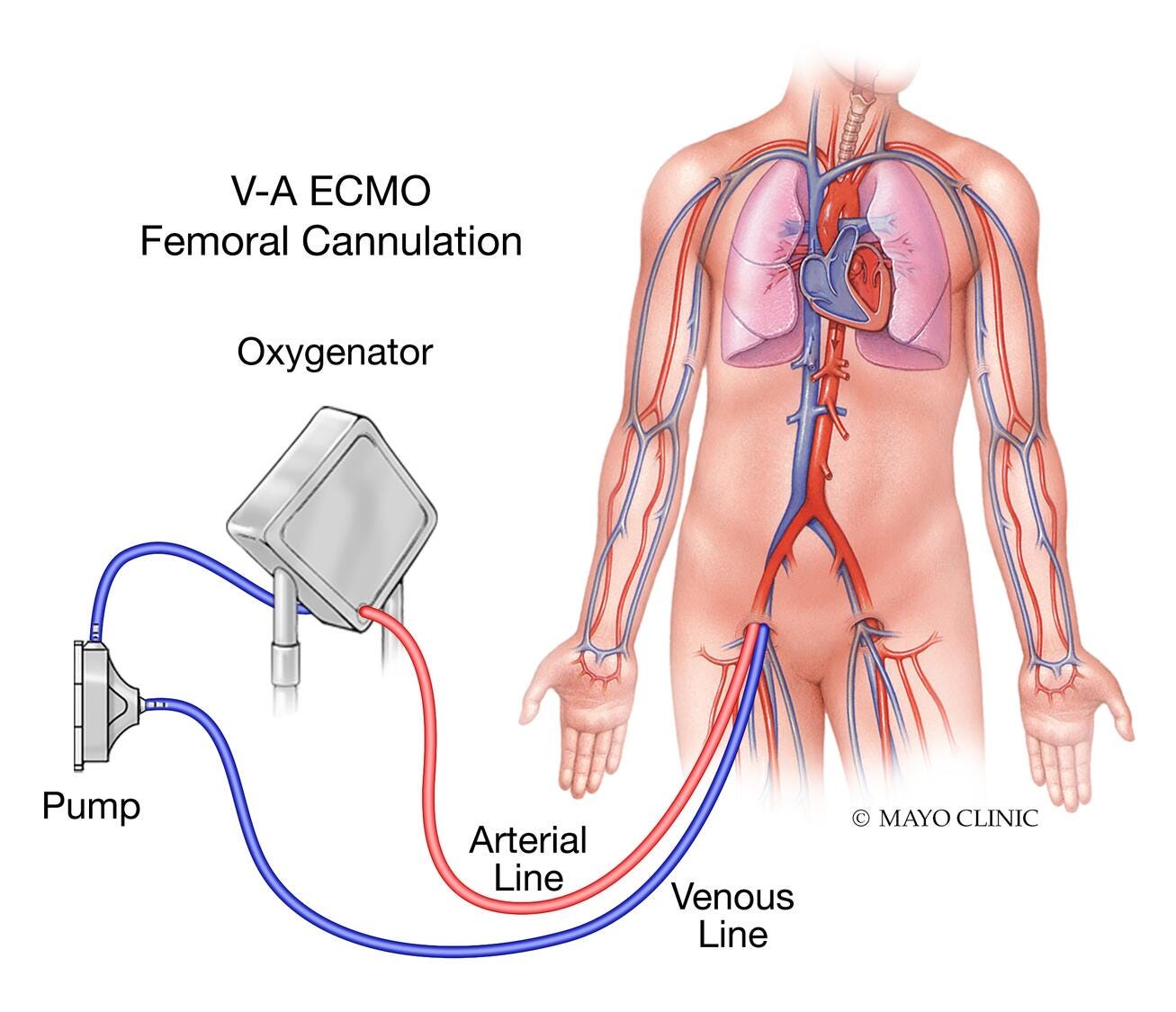
Veno-Arterial (VA) ECMO: Supports both heart and lung functions by returning oxygenated blood directly into the arterial system.
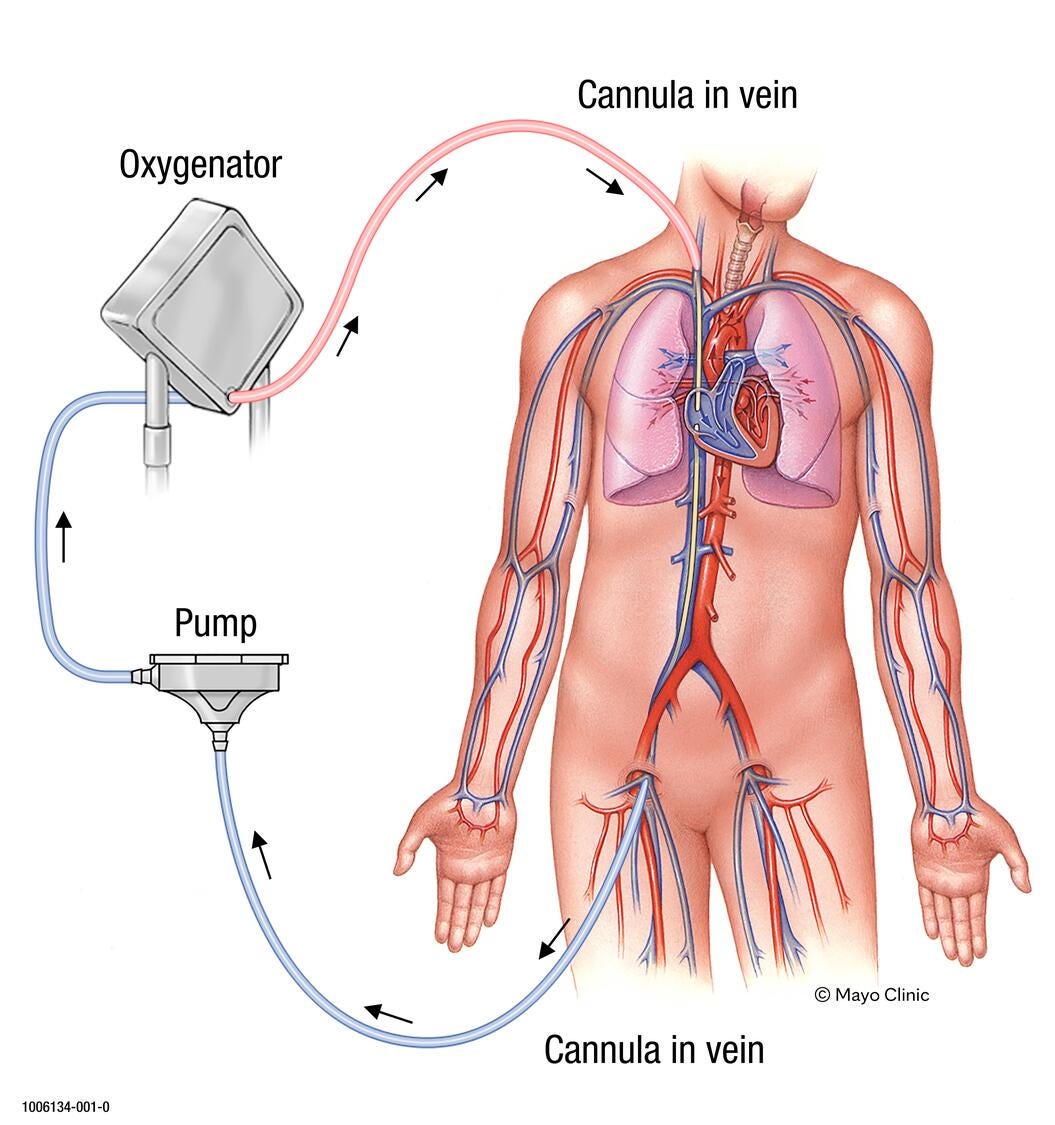
Veno-Venous (VV) ECMO: Supports only lung function by returning oxygenated blood to the venous system.
When is ECMO Used?
ECMO is considered in critical situations where the heart and/or lungs are severely compromised, such as:
Severe Respiratory Failure: Conditions like Acute Respiratory Distress Syndrome (ARDS) where the lungs cannot provide adequate oxygenation despite mechanical ventilation.
Cardiogenic Shock: When the heart is unable to pump sufficient blood to meet the body's needs, often due to heart attacks or severe heart failure.
Post-Cardiac Surgery: To support patients whose heart function is slow to recover after surgery.
Severe Infections: Such as pneumonia or COVID-19, leading to acute respiratory failure.
Bridge to Transplant: If the heart or lungs are too weak, then the patient can be placed on ECMO until the organ is available.
It's important to note that ECMO does not treat the underlying disease but provides critical support, offering time for other treatments to work or for the organs to heal.
Duration of ECMO Support
The length of time a patient remains on ECMO varies based on the underlying condition and individual response to treatment. Some patients may require ECMO for a few days, while others might need support for several weeks. Continuous monitoring and regular assessments are conducted to determine the appropriate time to wean a patient off ECMO.
Potential Risks and Complications
While ECMO can be life-saving, it carries potential risks, including:
Bleeding: Due to the need for blood thinners to prevent clotting in the circuit.
Infection: As with any procedure involving large blood vessels and external equipment.
Blood Clots: Which can lead to stroke or other complications.
Organ Damage: Such as kidney or liver injury from reduced blood flow or oxygenation.
Given these risks, ECMO is typically utilized when the potential benefits outweigh the possible complications.
Conclusion
ECMO is a complex, resource-intensive therapy reserved for patients with life-threatening heart and lung conditions unresponsive to conventional treatments. It requires a multidisciplinary team of specialists to manage the therapy and address any complications. For patients and families facing ECMO therapy, understanding its purpose, process, and potential risks can help in navigating this challenging aspect of critical care.
Learn more
If you want more ECMO breakdowns like this, make sure you are subscribed to this newsletter, ECMO 143: A Patient & Family Guide. In addition to my newsletter, organizations like the Extracorporeal Life Support Organization (ELSO) offer comprehensive guides for patients and families.
As a family member or concerned friend, one of the most helpful things you can do is be present during daily rounds if your hospital allows it. That’s when the care team reviews the plan and shares updates. Listen, take notes, and ask questions. You can also ask the nurse, ECMO specialist, or physicians to explain things in simpler terms. Most are willing to help. Timing matters. Try to ask when things are calmer so they can give you their full attention.